1️⃣ Introduction
Rational prescribing of medicines is a cornerstone of safe and effective clinical practice. Inappropriate medication use contributes significantly to antimicrobial resistance, preventable adverse drug reactions, unnecessary healthcare costs, and poor patient outcomes. Every prescription written by a clinician carries both therapeutic potential and responsibility. Practicing rational prescribing ensures that patients receive the most appropriate medication, tailored to their clinical condition, while minimizing risks and avoiding waste. This article explores the principles of rational prescribing and how clinicians can apply them in everyday medical practice.
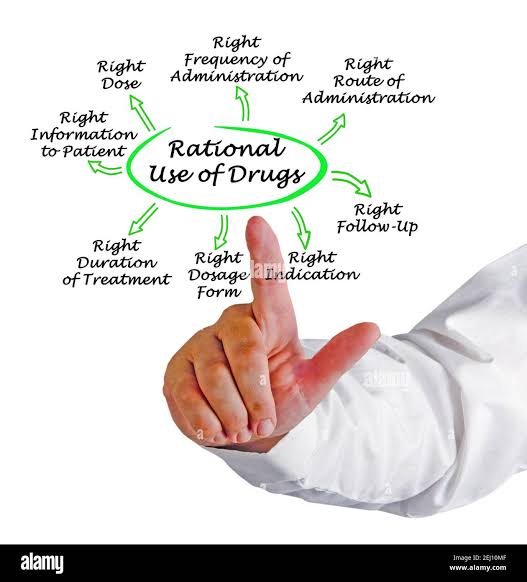
What is Rational Prescribing of medicines
Rational prescribing refers to the process of selecting and using medicines appropriately to achieve the best possible outcomes for patients. It involves:
Selecting the right drug
For the right patient
At the right dose
For the right duration
At the lowest cost to both the patient and the community
This approach requires careful clinical judgment, evidence-based decision-making, and consideration of patient-specific factors such as age, comorbidities, allergies, pregnancy status, and potential drug(medicines) interactions. prescription of medicine is not merely about treating symptoms—it is about providing safe, and effective medicines and toward individualized care.
Common Problems in Clinical Practice That Affect Rational prescribing of medicines
Despite its importance, irrational prescribing remains common in many healthcare settings. Some frequent challenges include:
Overprescribing antibiotics:
Unnecessary antibiotic use contributes directly to antimicrobial resistance, making infections harder to treat in the future.
Polypharmacy in elderly patients:
Multiple medications increase the risk of drug interactions, adverse effects, and poor adherence.
Incorrect dosing:
Underdosing may lead to treatment failure, while overdosing increases toxicity risk.
Failure to review medication history:
Not checking previous prescriptions can result in duplication, harmful interactions, or allergic reactions.
Patient pressure Affecting Rational prescribing of medicines:
Some patients expect prescriptions even when not clinically indicated, which may influence prescribing behavior.
Recognizing these issues is the first step toward improving practices toward prescribing medicines.
Practical Steps for Clinicians Toward Rational Prescribing Of Medicines
Improving prescribing requires consistent and structured clinical habits. The following steps can enhance safe prescribing:
Take a thorough history:
Always obtain a detailed medical, medication, and allergy history before prescribing.
Confirm the diagnosis:
Confirm the diagnosis:
Avoid prescribing without adequate clinical evaluation or diagnostic confirmation.
Use standard treatment guidelines
Follow national or international clinical guidelines to ensure evidence-based therapy
Review medications regularly
Reassess ongoing treatments, especially in chronic disease management and elderly patients
Educate patients:
Explain the purpose, dosage, duration, and possible side effects of medications to improve adherence and outcomes.
By integrating these practices into daily clinical work, healthcare professionals can significantly reduce medication-related harm
Conclusion
Rational prescribing is not just about choosing drugs—it is about protecting patients and preserving the effectiveness of medicines for future generations. Thoughtful, evidence-based prescribing improves patient safety, enhances therapeutic outcomes, and reduces the global burden of antimicrobial resistance. Every prescription should reflect careful clinical reasoning and a commitment to responsible medical practice.
Related Articles
- Dry Cough: Causes and Treatment
- Asthma Symptoms: Causes and Diagnosis
- Pneumonia Symptoms: Diagnosis and Treatment
- Tuberculosis Symptoms: Causes and Treatment